What the Best Disability Support Worker Apps Actually Include
A clear-eyed look at what a disability support worker app needs to do to be useful in the field — and why most generic workforce apps fall short for NDIS providers.
What a Disability Support Worker App Actually Needs to Do
The appeal of a "disability support worker app" is obvious: support workers spend their days in the field, not at a desk. Their tools need to be on their phone.
But most workforce apps were not built for disability support. They were built for hospitality, retail, or construction — and then described as suitable for care. The gaps show up quickly once workers start using them.
This article covers what a disability support worker app actually needs to include to be useful in NDIS-funded services, and how to evaluate what is on the market.
The core job: get the worker to the visit prepared
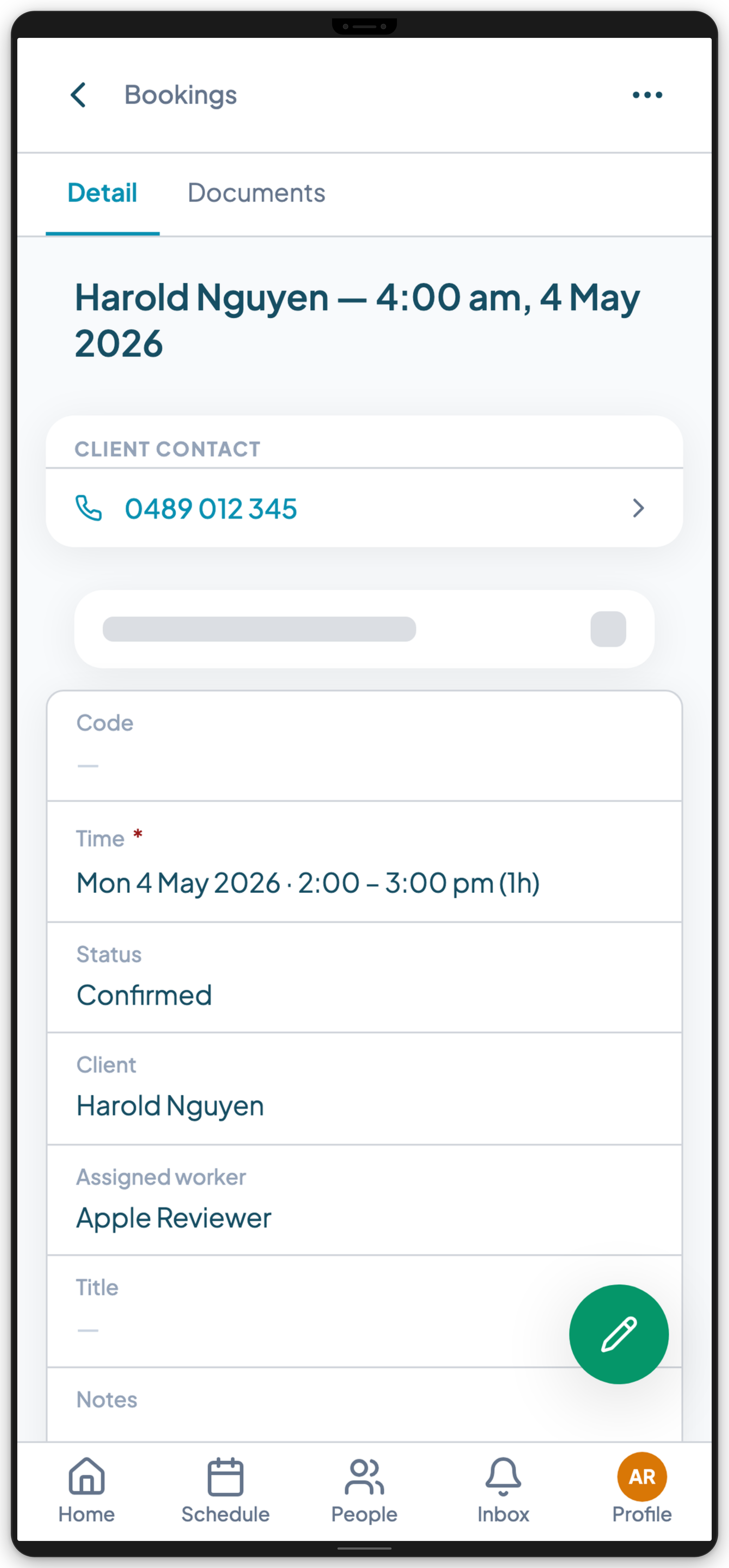
Before anything else, the app needs to answer one question: what does this worker need to know before they knock on the door?
For a disability support worker, that means:
The participant's name, address, and access instructions. Not just a name in a schedule — the actual address, any gate codes or building entry notes, and how to get there if the address is unusual.
Support plan context. What supports are scheduled for this visit? What does the participant's NDIS plan say about how they want to be supported? What are their preferences, routines, and communication style?
Health alerts. Any conditions the worker needs to know before they arrive — allergy and anaphylaxis alerts, mobility and manual handling requirements, communication needs, and pointers to the care plan, behaviour support plan, or PRN protocols where relevant.
Recent visit history. What happened at the last few visits? Was the participant unwell? Did anything significant occur? A support worker arriving cold — with no context from the previous shift — is a worse worker, not because of capability but because of information.
A generic rostering app shows a name and a time. A disability support worker app shows everything the worker needs to do their job properly.
GPS check-in and check-out
NDIS providers need to be able to demonstrate that services were delivered as agreed. GPS check-in does three things at once: it confirms the worker arrived, records the time, and creates a location-stamped record that holds up to scrutiny.
This matters for:
- Payroll accuracy. Recorded check-in and check-out times reduce timesheet disputes. Workers are paid for what they worked; providers are not paying for time that was not delivered.
- NDIS audit readiness. When the NDIS Quality and Safeguards Commission asks for evidence that services were delivered on a specific date for a specific participant, GPS check-in records are part of that evidence.
- Participant safety. If a worker checks in but then does not check out within an expected window, that is a signal that something may be wrong.
Generic apps that record check-in without GPS are significantly less useful for NDIS compliance purposes. Location confirmation is not a nice-to-have.
Shift notes in the app, not on paper
Every NDIS provider has an obligation to maintain records that demonstrate services were delivered and that workers observed and responded to participant needs. Shift notes are the primary mechanism for this.
Shift notes submitted in the app immediately after a visit are:
- More accurate. The worker fills them in while the visit is fresh, not hours later from memory.
- Immediately accessible. Coordinators can read them in real time, not when a paper form turns up at the office.
- Linked to the correct record. Notes submitted through the app attach to the participant, the shift, the worker, and the date automatically. There is no transcription step and no risk of misfiling.
- Structured. A good app guides the worker through what to record rather than presenting a blank text field. Structured notes are more consistent and more useful.
The difference between a shift note submitted at 3:15pm from the participant's living room and one reconstructed at 8pm from memory is significant — both in accuracy and in what it demonstrates about the provider's practice.
Incident reporting from the field
NDIS providers have mandatory reportable incident obligations. Some incidents must be reported to the NDIS Commission within 24 hours, with a detailed follow-up report required within 5 business days. Internal documentation requirements are broader still.
An incident that is reported from the app immediately after it occurs is documented while the facts are clear and the worker is still on site. An incident that gets reported two days later, reconstructed from a phone call, is a problem for several reasons: the facts may be less accurate, the timeframe may not comply with reporting obligations, and the documentation may not be complete.
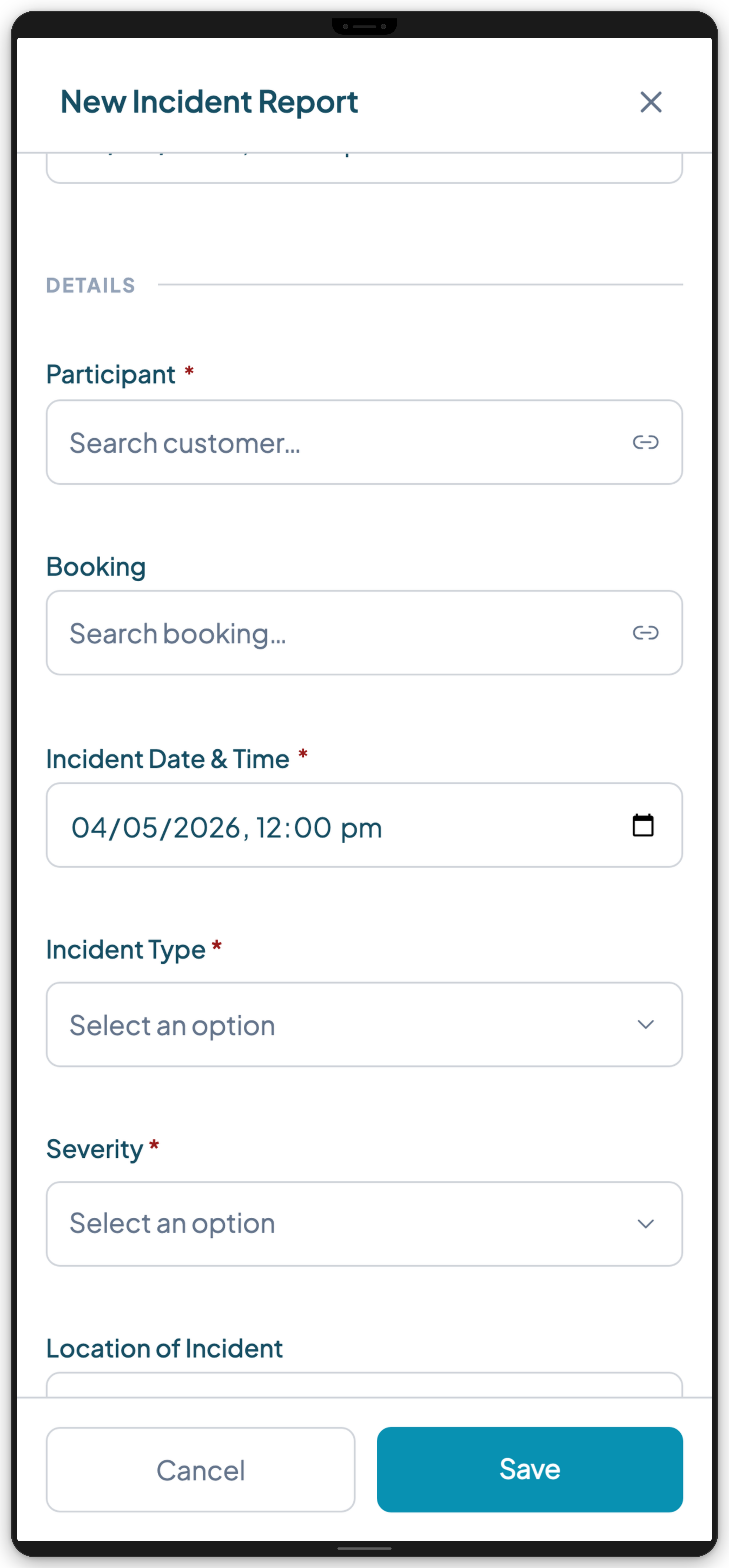
The best disability support worker apps include structured incident reporting with:
- Mandatory fields that ensure nothing is missed
- The ability to attach photos or documents
- Automatic linking to the participant, shift, and worker
- Immediate notification to the coordinator
- Automatic timestamp on submission; GPS location optional where appropriate.
Communication with coordinators, in one place
Support workers in disability services communicate with their coordinators constantly: availability changes, questions about a participant, shift swap requests, incident updates, concerns about care.
This communication happens across WhatsApp, SMS, phone calls, and email — and none of it is recorded in any useful way. When a coordinator leaves, or when a new worker starts, the context is gone.
A support worker app that includes a communications channel — messages logged against the participant or the worker record, visible to all coordinators with appropriate access — solves a problem that most providers do not realise is costing them significantly in administrative overhead and care continuity.
What generic workforce apps miss
The most common alternatives to care-specific apps are:
Deputy, Humanforce, Roubler. Built primarily for hospitality, retail, and warehousing, with care providers as a secondary use case. Scheduling and timesheet features are solid; participant records, NDIS compliance tracking, structured shift notes, incident reporting, and care plan context for workers are not native.
WhatsApp + spreadsheets. Where most providers start. Works at very small scale. Fails badly as complexity grows: no audit trail, no compliance tracking, no search, no structure.
Generic task management apps (Asana, Monday, etc.). Not built for shift-based care at all. Require significant customisation to approximate a rostering function, with none of the NDIS-specific features.
Teiro. Built for Australian disability support, aged care, and community health providers. Workers use the iOS or Android app for their daily schedule, GPS check-in, shift notes, incident reports, and coordinator messages. Coordinators use the web platform and mobile app for rostering, credential tracking, participant records, and compliance monitoring.
Evaluating an app for your team
When comparing options, ask:
- 1.Can workers see participant support plan details on their phone before a shift?
- 2.Does check-in capture GPS location?
- 3.Are shift notes submitted in the app and immediately accessible to coordinators?
- 4.Is incident reporting built in, structured, and linked to the participant record?
- 5.Does the rostering system track worker credentials and flag mismatches?
- 6.Is the app built for Australian NDIS requirements, or adapted from a generic workforce tool?
An app that cannot answer yes to all six is filling some of your needs but not all of them. The gaps tend to be covered by WhatsApp, spreadsheets, and phone calls -- which is where compliance and care quality problems originate.
Teiro is free for organisations with 5 or fewer active users. Book a demo at teiro.com.au/demo or sign up at teiro.com.au/signup.
Related reading: Best NDIS apps in Australia 2026, GPS check-in for NDIS carers, How to check in to a shift on Teiro.